Sleep Coaching Is Now a Recognized Treatment in the US — What That Actually Changes
For years, the conversation around sleep in wellness and fitness circles stayed frustratingly soft. Coaches offered tips. Apps tracked hours. Articles repeated the same advice about blue light and bedroom temperature. None of it carried clinical weight, and none of it gave practitioners a legitimate framework to work within.
That's changing. In 2026, the American Academy of Sleep Medicine (AASM) formally recognized behavioral sleep coaching as a valid treatment approach for chronic insomnia, extending non-pharmacological options beyond the clinical boundary of CBT-I delivered by licensed therapists. The implications for coaches, athletes, and wellness professionals are significant — not because sleep science changed, but because the institutional framework around it did.
What the AASM Recognition Actually Means
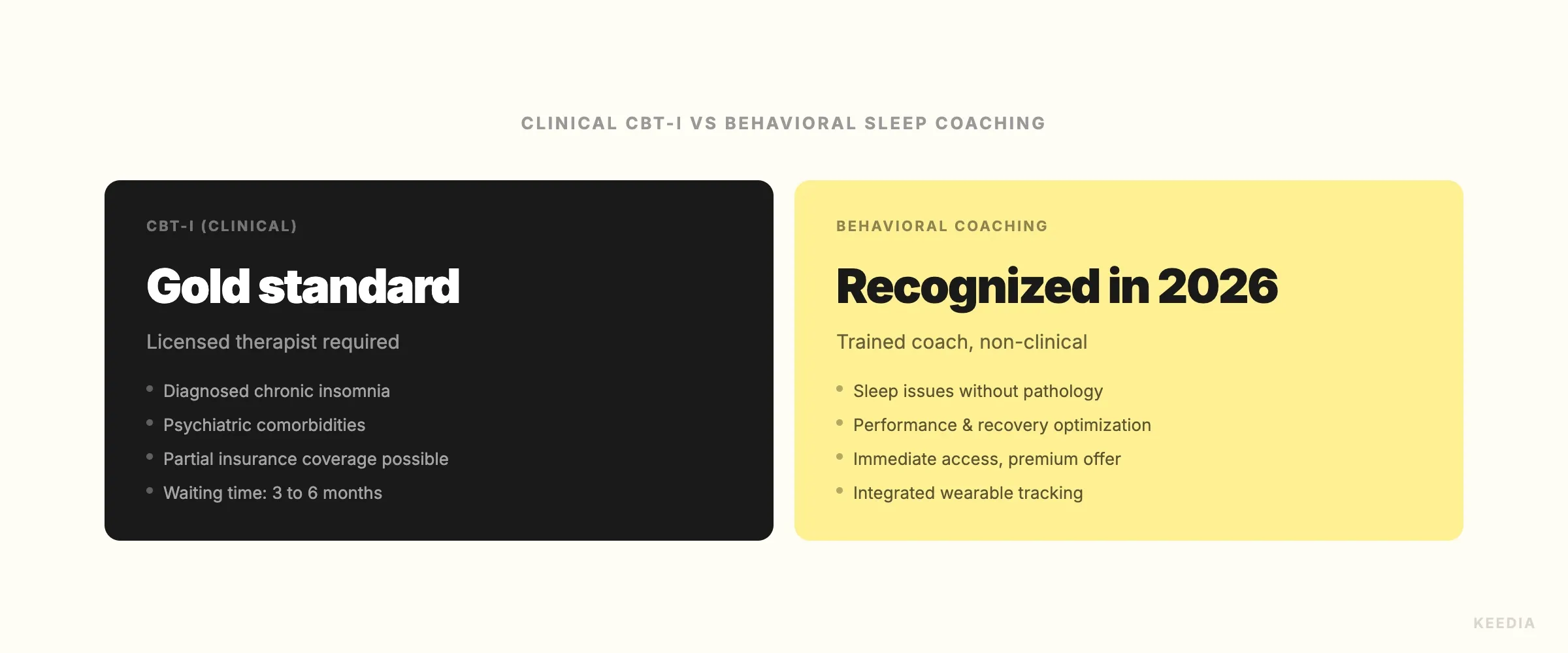
Cognitive behavioral therapy for insomnia (CBT-I) has long been the gold standard for treating chronic sleep disorders without medication. It's effective, well-researched, and delivered by licensed mental health professionals or sleep specialists. The problem is access. Waitlists for qualified CBT-I practitioners can stretch months, costs run high, and the majority of people struggling with sleep quality don't meet the clinical threshold for a formal insomnia diagnosis in the first place.
The AASM's updated position recognizes that a structured behavioral approach, delivered outside the clinical setting, can meaningfully address sleep disturbance in this broader population. This isn't a relaxation of clinical standards. CBT-I remains the appropriate intervention for diagnosed clinical insomnia. What's changed is that non-clinical practitioners now have a recognized framework to work within, with defined protocols and a clear scope of practice.
That's a meaningful institutional shift. It moves behavioral sleep work from "wellness advice" into structured, legitimized practice.
What Behavioral Sleep Coaching Actually Involves
This is where the distinction from generic sleep hygiene content matters. Behavioral sleep coaching isn't a checklist of bedroom tips. It's a structured set of interventions drawn from the same evidence base as CBT-I, applied in a non-clinical context.
The core components include:
- Sleep hygiene restructuring: Not a list of rules, but an individualized audit of behaviors, schedules, and environmental factors that are actively disrupting sleep architecture.
- Stimulus control therapy: Systematically rebuilding the mental association between bed and sleep, rather than wakefulness or anxiety. This is one of the most effective single interventions in insomnia research.
- Sleep restriction protocols: Temporarily limiting time in bed to consolidate sleep efficiency before gradually extending it. Counterintuitive, moderately uncomfortable, and highly effective for building sleep drive.
- Sleep scheduling and circadian alignment: Anchoring wake times, managing light exposure, and structuring the day to support natural sleep pressure.
These are protocols with measurable outcomes, not suggestions. That's the point. Coaches who operate within this framework are doing structured behavioral work, not lifestyle consulting.
What This Opens Up for Coaches and Fitness Professionals
If you're a certified wellness coach, personal trainer, or health professional, the AASM recognition creates a legitimate service category you can now offer with institutional backing. Sleep optimization as a paid service, built around behavioral protocols and objective tracking, is no longer operating in a gray area.
The scope of practice boundaries remain clear: you're not diagnosing, you're not treating clinical disorders, and you're not delivering therapy. If a client presents with symptoms that suggest a clinical condition, including sleep apnea, restless leg syndrome, or severe clinical insomnia, the appropriate step is a referral to a medical provider. Behavioral sleep coaching serves the large population of people who are sleeping poorly but don't meet clinical criteria.
That population is substantial. Survey data consistently shows that between 30 and 40 percent of adults in the US report insufficient sleep quality, while clinical insomnia prevalence sits around 10 to 15 percent. There's a large middle ground of people with real, disruptive sleep problems who aren't candidates for clinical treatment but would benefit from structured behavioral intervention.
From a business standpoint, this adds meaningful service depth. Sleep coaching can function as a standalone offering, typically priced between $150 and $350 per month for structured programming, or as an integrated component of a broader health and performance package. If you're already thinking about pricing psychology and how structured services justify higher rates, sleep coaching is a strong example of a high-value, evidence-backed addition that supports premium positioning.

Wearables Have Changed the Data Layer
One of the reasons behavioral sleep coaching is now viable at scale outside clinical settings is the data infrastructure that consumer wearables have built. Devices like Oura, WHOOP, and Fitbit now track HRV, sleep stage distribution, respiratory rate, and resting heart rate with enough consistency to support behavioral coaching conversations that weren't possible five years ago.
This matters because it transforms sleep from a subjective experience into a trackable variable. A client who says "I'm sleeping badly" can now show you a week of HRV suppression, fragmented deep sleep staging, and elevated resting heart rate that confirms physiological stress. That data gives you something to work with, and it gives the client objective feedback on whether behavioral changes are producing measurable results.
It's worth being honest about limitations. Consumer wearables are not clinical-grade polysomnography, and sleep stage accuracy in particular varies across devices and individuals. But for trend tracking and behavioral feedback loops, the data layer is genuinely useful. Coaching decisions shouldn't be based on a single night's readout, but week-over-week pattern changes are informative.
For clients also managing nutrition protocols, sleep data intersects meaningfully with recovery metrics. If you're working with someone on magnesium supplementation to support sleep quality, wearable data can help you assess whether the intervention is shifting sleep architecture in the right direction.
What This Means Specifically for Athletes
For athletes and performance-focused clients, the institutional recognition of sleep coaching closes a gap that has existed in performance programming for years. Sleep has always been acknowledged as important. What's been missing is a structured, protocol-based approach that sits alongside training, nutrition, and recovery in a periodized plan.
That's now available. Sleep optimization as a performance variable means you can assess a client's sleep quality at baseline, identify the specific behavioral drivers of disruption, implement structured interventions, and track objective outcomes over time. That's a performance protocol, not a wellness tip.
For athletes in heavy training blocks, the intersection with recovery is direct. Sleep restriction and sleep fragmentation both impair HRV, increase cortisol, reduce glycogen resynthesis, and compromise motor learning. Research consistently links insufficient sleep to higher injury rates and longer recovery windows. The protocols used to improve aerobic capacity don't work as intended when sleep is chronically compromised.
Sleep coaching adds another layer to the recovery conversation that already includes modalities like cold water immersion and contrast therapy. Unlike those tools, behavioral sleep coaching addresses the primary recovery mechanism directly, not a supplementary one.
Where CBT-I and Behavioral Coaching Fit Together
It's worth being precise about the distinction, because conflating the two creates scope of practice problems. CBT-I is a structured psychological treatment with a defined clinical protocol, typically delivered over six to eight sessions by a licensed provider. It includes cognitive components targeting maladaptive beliefs about sleep that are outside the scope of behavioral coaching.
Behavioral sleep coaching draws from the behavioral components of CBT-I but doesn't include the cognitive therapy elements. It's the appropriate intervention for subclinical sleep problems in otherwise healthy adults. Think of it the way you think about the relationship between a registered dietitian and a certified nutrition coach: different scope, different depth, different clinical authority, but both legitimate and both useful for different populations.
The referral pathway matters. A sleep coach who identifies a client with symptoms of sleep apnea, chronic depression affecting sleep, or severe clinical insomnia needs to direct that client to appropriate medical care. Staying within scope isn't a limitation of the service. It's what makes the service credible and safe.
The Practical Takeaway for Practitioners
If you're a fitness or wellness professional looking to expand your service offering in a direction that's evidence-backed, institutionally recognized, and genuinely underserved, behavioral sleep coaching now has a framework that supports it. The AASM recognition gives you a professional foundation, consumer wearables give you a data layer, and the demand is demonstrably there.
That said, approach it with the same rigor you'd apply to any structured coaching methodology. Getting proper training in behavioral sleep protocols matters, both for client outcomes and for your professional credibility. The recognition legitimizes the category. What you do within it still depends on your competence and your commitment to staying within defined scope.
Sleep is no longer a soft wellness topic that sits outside structured programming. It's a performance variable with measurable outcomes, recognized protocols, and a legitimate place in the work you do with clients. That's the shift worth paying attention to.
